TOC & Search | Palm
Index | Rx | Pt. Ed UC
| PubMed | Refs | Disclaimer | Home
- open vs. closed
- location (shaft, intra-articular)
- displacement in mm
- shortening in mm
- impaction if present
- angulation, degree and direction (midshaft - direction of apex, end - direction of
terminal fragment)
- Salter classification (pedes)
| Indication |
View |
| sternoclavicular subluxation |
cephalic tilt |
| clavicle (medial) |
AP and 45 degree cephalic tilt or apical lordotic |
| AC separation |
weighted |
| glenohumoral separation |
true lateral |
| shoulder dislocation, ant |
axillary |
| shoulder dislocation, post |
true lateral |
| scaphoid fx |
navicular view |
| neck trauma |
C-spine series |
ref: Commonly Missed Orthopedic
Problems AFP 1998: Anterior cruciate, slipped
capital femoral epiphysis, femoral neck stress fracture, scaphoid
fracture, UCL/Gamekeeper’s Thumb, achilles tendon,
posterior tibial tendon rupture.
All
- neurovascular compromise: esp with dislocation of shoulder, tibiofemoral
Pediatric
- Monteggia fracture: fracture of ulna (mid) with anterior
dislocation of head of radius. See loss of passive supination at the elbow. X-ray both
elbow and wrist. Refer.
- Buckle fracture of distal radius: no deformity, normal passive but not active motion.
Wrist ext. & forearm pro/sup -> pain. Point tenderness 1.5” proximal to the
wrist. X-ray shows buckle fracture: very hard to see. Heals well, but should splint.
- spiral fracture of tibia: minimal findings, but child who is afebrile and refuses to
walk and has normal joint exams. Bone scan or 45 degree oblique x-ray may show fracture.
Immobilize in cast for 3-4 weeks. Child abuse considered.
Galeazzi Fracture
radius fracture with radioulnar dislocation. Wrist tender. Lateral wrist may show
dorsal angulation of radius compared to ulna.
midfoot-forefoot disruption: compartment syndrome from loss blood supply to forefoot.
Massive swelling can be seen. Subtle x-ray, need comparison film to see 1st-2nd metatarsal
shaft widening or proximal shift of 5th metatarsal base.
Ref: Lisfranc Injury of the Foot
- July 1998 - AFP
See also Osteoporotic vertebral fracture (compression).
Common Errors
- reliance on x-ray rather than exam.
Salter Classification (pedes)
- separate epiphysis from metaphysis. Good prognosis. Seen most commonly in birth
injury.
- along epiphysis then out through metaphysis. Most common of all fractures, age
often > 10. Reduction -> good prognosis.
- intra-articular, from joint space through epiphyseal plate, then to periphery.
Good prognosis if surgical repair or if excellent closed reduction. Usually a fracture of
the distal tibial epiphysis, see Tillaux fracture.
- intra-articular, from joint space through metaphysis. Growth arrest
common, open repair.
- compression of epiphyseal plate. Not seen on x-ray. Uncommon. Suspect if
persistent pain/compression mechanism and negative film.
Facial, orbital and related
- Zygomatic arch: trismus, left periorbital swelling, usually tripod with TMJ pain
- Inferior orbit: numbness of cheek (infraorbital nerve), may have limited upward gaze
- medial orbit: blowout fracture, limitation of abduction
- basal skull: racoon eyes
- nasal fracture: beware nasal septal hematoma -> necrosis septal cartilage
See: Cervical spine series. Rx: methylprednisolone 30
mg per kg IV over 1 hour then 5.4 mg/kg per hour
| Spine level |
Fracture name |
Stable or unstable |
Mechanism/clinical setting |
Radiologic findings |
| C1 |
Jefferson fracture (Figures 6 and 7) |
Moderately unstable |
Burst fracture; occurs with axial load or
vertebral compression |
Displaced lateral aspects of C1 on odontoid
view, predental space more than 3 mm |
| Atlantoaxial subluxation |
Highly unstable |
Occurs in patients with Down syndrome,
rheumatoid arthritisand other destructive processes |
Asymmetric lateral bodies on odontoid view,
increased predental space |
| C2 |
Odontoid fracture (Figures 1 and 9) |
Highly unstable |
Mechanism poorly understood |
May be difficult to see on plain films; high
clinical suspicion requires CT scanning |
| Hangman's fracture (Figure 8) |
Unstable |
Occurs with sudden deceleration (hanging)
and with hyperextension, as in motor vehicle accidents |
Bilateral pedicle fracture of C2 with or
without anterior subluxation; lateral view required |
| Any level |
Flexion teardrop injury |
Highly unstable |
Sudden and forceful flexion |
Large wedge off the anterior aspect of
affected vertebra; ligamentous instability causes alignment abnormalities |
| Bilateral facet dislocations |
Highly unstable |
Flexion or combined flexion/rotation |
Anterior displacement of 50% or more of one
cervical vertebra on lateral views |
| Unilateral facet dislocations (Figure 5) |
Unstable |
Flexion or combined flexion/rotation |
Anterior dislocation of 25 to 33% of one
cervical vertebra on lateral views; an abrupt transition in rotation so that lateral view
of affected vertebra is rotated; lateral displacement of spinous process on
anteroposterior view |
| Lower cervical or upper thoracic |
Clay shoveler's fracture |
Very stable |
Flexion, such as when picking up and
throwing heavy loads (such as snow or clay) |
Avulsion of posterior aspect of spinous
process; frequently an incidental finding |
| Cervical
Spine Radiographs in the Trauma Patient - January 15 1999 - AAFP |
Clavicle
middle third - management
- restrict shoulder motion to < 45 degrees abduction. Pt needs to tighten figure-of-8
splint regularly, use arm slign. Immobilize to no tenderness/crepitus over fracture site.
Elbow ROM.
- clinical union 6-12 wk (3-6 child), x-ray 12 wk. Do final film. Avoid reinjury 2-3
months
distal third - management
- look like AC separation. May require stress films to see or even MRI (fracture through
AC joint)
- Type II has AC ligs attached to distal part, proximal goes upwards. Needs referral. Immobilize.
proximal third
- 45 degree cephalic tilt
- treat with sling, heal 6-8 weeks.
Humeral head
Immobilize arm against chest for 6 weeks. Start ROM ex. at 3 weeks. If young and only
piece off surgery. ALWAYS test pinch (ulnar) and
sensation (median).
Elbow (pediatric)
- 67% supracondylar (axial loading with locked elbow). Posterior fat pad may be only sign.
- 17% lateral condylar: need oblique views. Suspect when lateral side elbow sore/swolllen.
Growth arrest.
- always do comparison views
- order 3 views: AP, lateral, and internal oblique (supinate palm)
- line drawn down anterior surface of radius should bisect capitellum on lateral view
- capitellum ossification 1-2 yrs, radial head 3-5, olecranon 9-10
- neurovasc: pulses, hand temp, refill, nerves
- immobilize at 70° (90° may compress brachial artery)
Wrist
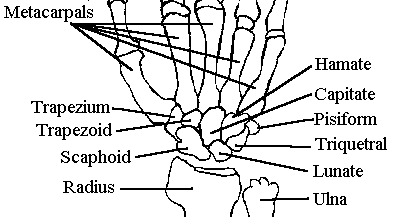
Inspection X-ray
- AP: radius and radial styloid, ulnar and ulnar styloid, navicular (most common fx),
metacarpal base
- lateral: alignment of radius, lunate, capitate - line from radial shaft pass through
middle of lunate, capitate
Scaphoid (Navicular) Fractures: fall on the outstretched hand
- most common wrist fracture
- pain, swelling, very tender snuff box
- cast/splint immobilization and repeat radiographs 2-3 weeks post-injury. If not fracture
but markedly tender recheck in 3-4 weeks. If better then remove splint. (Fracture requires
up to 3-4 months in cast.)
Reduction
If reduce use 8-10 ml .25% marcaine at fx site, apply trcn to medial side of thumb and
finger, then restore angle. Keep up in air with splint before casting (dec. swelling).
Short arm cast must end proximal to distal metacarp-phalangeal joint. Warn pt: WILL LOSE
MOTION. Get AP, lateral, and oblique navicular view -- if snuff box tender splint x 2w, if
still tender re x-ray, if nec. do bone scan.
Fingers and thumb
- Mallet finger: avulsion of extensor tendon from distal phalanx. Unable to extend DIP. --
splint in extension x 6-8w. If fx metacarp-phalang immobilize in flexion.
- Dislocation -- reduce in ER, test collateral lig. If dorsal dislocn splint bent 15 deg.
& flexd for 2w. If ventrl splint straight.
1st MCP ulnar collateral ligament
strain: forced abd and ext. Ulnar
collateral ligament is on dorsal side of MCP when hand is flat on table. R/O fx, then
stress test positive if 20 deg more radial (dorsal) deviation than other side.
Immobilize with Spica cast or thumb splint in 30 degree flexion for 4-6 week, with
active ROM at 3-4 weeks. If healing then can use a tape loop from thumb to index
finger to prevent abduction, extension of thumb. Refer if associated fracture or large
deviation on stress test.
Hip
Ankle & Foot
- Jones fx is most common - proximal 5th metatarsal. High incidence non-union.
- Snowboarder's Ankle: Fracture of lateral process of talus. Rare outside snowboarding.
Risk avascular necrosis. Look on mortise view distal lateral malleolus with foot
internally rotated. Consider if "sprain" does not respond -> CT.
- Salter III or above
- clavicle: distal third
- humerus: > 1 cm displacement or rotation/angulation > 33 degrees, mid-shaft
fracture especially
- radial head: Type II - large articular surface > 30% fragmented or > 3 mm
displacement. If elbow dislocation high risk urgent neurovascular compromise.
- ulna: > 50% displacement nightstick fracture, unstable or not isolated
- wrist: anything but a nondisplaced nonangulated Colles fracture that can be reduced to
neutral position or slight posterior inclination. Dislocation of carpal bones requires
immediate orthopod exam.
- proximal phalanx, intra-articular
- scaphoid: any complicated fracture.
- femur: anything but an isolated fracture of greater trochanter
- patella: an unstable or displaced fracture that prevents patient doing a straight leg
raise
- fibula: nonisolated or unstable fractures
Shoulder (see views)
Anterior
- hold in adduction with slight internal rotation, hollow glenoid, can palpate head along
anterior axillary fold
- check axillary and muculotendinous nerves and
radial pulse
- reduce: external rotation, pt. face up, elbow on bed. Abduct to 90°, gentle traction. Obtain
post-reduction film
Posterior
- can't abduct the shoulder at all! Easy to miss ...
- pull with arm extended or hyperextended
- dislocates anteriorly, usually arm partly flexed
- bilateral x-ray and neurovascular exam first
- warn parents, will hurt for a moment
- supinate and fully flex, then gently extend, thumb on radial head
- recheck in 5 minutes for function
Finger: MCP
- proximal phalanx usually dorsal, results from forced hyperextension
- signs may require open reduction (complex dislocation):
- MP joint only slightly hyperextended (usually is 90 deg)
- palmar dimple (volar plate attached to palmar tissue)
- widened joint space on x-ray (interposed tissue)
- sesamoid bone in jt space (pathognomic, sesamoid part of volar plate)
- if simple dislocation, can reduce. Use wrist block. NO TRACTION. Flex
DIP and PIP and wrist & hyperextend MP to 90 deg, maintain contact between prox
phalanx and metacarpal, and push forward into place, then gently flex. Splint in mild
flexion and refer for f/u.
- PIP dorsal dislocation: immobilize in gentle flexion for 2-3 weeks
- PIP volar dislocation middle phalanx: check no boutonniere deformity (avulsion
extensor from base of middle phalanx) Some hand surgeons will do primary repair
immediately.
- lunate is most frequently dislocated hand bone, 2nd most common fx.
Patella (lateral dislocation)
- ref: Functional
Treatment of Patellar Dislocation in an Athletic Population ($)
- medial dislocation: contact orthopedics
- lateral occurs when foot planted, bearing wt, knee flexed, valgus, and externally
rotated.
- confirm by displace patella laterally with knee flexed 30 deg, tenderness medial
retinaculum
- r/o coexistent ACL tear
- x-ray AP, lateral, tunnel of involved knee, Merchant view both knees
- arthrocentesis if large blood or knee persistently displaced
traditional mgt
- initial immobilization. Used to be immobilized for 7 weeks, newer protocols do earlier
rehab.
- surgery for atheletes.
early rehab (non-surgical)
- ice for 48 hours
- immediate straight leg raises, knee sleeve with lateral padding
- 3-8 weeks of quadriceps rehab
- 2/3 with initial subluxation good results at 2 years with conservative mgt. Results
worse in women, esp if bilateral laxity.
Back pain (and similar hip/bursa pains)
Diagnosis
- ask for history of CA, infection, prostate symptoms
- buttock and leg pain: if internal rotation of the hip is preserved significant DJD hip
is ruled out. (int. rotn. is 1st to go; sx of groin pain.).
- trochanteric bursitis: a treatable cause of pain referred to the back, groin or hip.
Worse with standing, better sitting.
- L5 lesion: weak extension of the great toe, loss of ankle jerk. L4: loss of knee jerk,
pain down shin, pain on ext. of hip. L3: loss of knee jerk, pain to knee.
meds
- flexeril 10 mg po tid (cntrl musc. rel. very similar to tricyclic adps.) or valium 2 or
5 mg tid.
- fiorinal 1-2 po q4h (325 mg asa + butalbitol [a barbiturate!] + caffeine), #3 (+30 mg
codeine).
- * - parafon forte 250-500 mg tid-qid. A sedative "muscle relaxant". NO
tylenol.
- motrin 400-600 mg tid-qid
- cochicine, both IV and PO, has been used for severe back pain. There are few references,
but it gets a "B" grade in back pain guidelines. Mechanism unknown.
ref: Ottawa
Rules
Hx and Exam
- Lachman test for ACL injury: Flex 15-30 deg., femur still, pull tibia anterior, feel for
solid thud of ligmt. If incr. motion, no thud, then torn.
- acute swollen knee
- bleeding into joint --> POP and swelling within 3 hours. ACL ruptured (women most
vulnerable). Lachman (Flex 15-30 deg., femur still, pull tibia anterior, feel for solid
thud of ligmt. If incr. motion, no thud, then torn.) pos; but usually cannot do well when
knee swollen. Need reconstruct -- do any time. Aspirate for pain control prn. D/DX
fracture, patellar dislcn (pain on latrl motion patella). "Segund" fracture:
avulsion lateral aspect proximal tibia
- meniscal tear --> slow modest effusion with diffuse tenderness. "POP" +
slow swelling + inability to extend knee --> arthroscopy. Intermediate effusion with
locking and medial jt line tenderness --> flap tear Rx Sx. (McMurray: knee and hip well
flexed, extend and stress altrnt sides while feel area of menisci. Degree of knee extnsn
at which click occurs is propt. to how far antr. tear is.)
- lateral collateral: test at 30 degrees flexion
- lots of MRIs done now, but unclear as to logic
- x-ray rules (fx): age>55, tender head fibula, isolated patellar tenderness, inability
to flex to 90deg, inability to bear weight both immediately and in UC. Recheck 5-7 days if
not better.
Therapy
- seven days of rehab for 1 day immobilization.
- medial collateral strain (gr 1-2): immobilize x 3 weeks?? (seems too long). If gr 1 can
use BCB brace (vi) and running after 2 weeks, wear brace x 3-5 weeks. If gr 2.0 no sports
until pain free. Gr. 3 (totally unstable) --> operate.
- medial meniscal tear: use McMurray test. Degree of extension of knee at which click
occuis propt. to how far anterior the tear is.
- severe abuction injury: complex. Tear deep and superficial medial ligament, medical
meniscus and anterior cruciate.
Deformities
- Mallet finger: flexion of DIP from avulsion of external tendon (splint in extension)
- Boutonniere: flexion of PIP, extension DIP from rupture central slip PIP. If suspect,
splint PIP only in full extension.
- Swan neck: hyperextension of PIP with flexion of DIP from RA, old mallet or PIP volar
plate injury
- Claw hand: hyperextension of MCP, flexion DIP/PIP from ulnar
nerve injury
- The Injured Ankle (AFP 1/98)
- subtalar joint does all the supination or pronation (normally), tibiofibular ligament is
critical to mortice stability
- peroneal tendon (longus mostly, also brevis) is a major contributor to stability,
prevents dynamic inversion
- forceful dorsiflexion or external rotation: talus separates tib-fib. Very forceful
inversion: talar dome fx.
- if "pop" then more significant ligamentous damage, prior ankle sprain: more
aggressive rehab
- anterior drawer useful (pull forward, backward) for severe disruption, squeeze test:
squeeze mid-lower leg, see if pain referred to interosseus structures, talar tilt not
useful, stress fractures rarely done
- Ottawa ankle rules (adults) x-ray ankle if:
- unable to bear weight both immediately and in ER
- bone tenderness over posterior distal 3 cm of lat/mid fibula
Therapy
- early range of motion even for fairly severe injury - do the alphabet
- NSAIDs may slow healing?
- grade III injuries: today less surgery, ankle stabilize devices rather than casting such
as sugar tong or heavy boot splint, refer to therapy for rehab
- nondisplaced lateral malleolus fracture (blow to malleolus): cast boot for 3 weeks.
- splint with AirCast initially then lace up stabilizer - laces should be .5-1"
apart, relace after initial use (Swedo) for long term.
- range of motion: pretty immediate
- progressive exercise: swimming, exercise bike, mini-tramp, Nordic track, walking,
gradual increase running, sport
- proprioception: balance on leg with eyes closed
- persistent pain, swelling months later -- talar dome
fracture.
- High-ankle sprain - syndesmosis talo-fib strain: 4-6 weeks of rehab
High ankle sprains - Syndesmotic
- football injury: dorsiflexion and eversion
- tear tib/fib ligaments and interosseous membrane -> chronic instability
- squeeze test: mid-calf tib/fib compression -> pain in anterior tib/fib ligament.
Other: external rotation stress test, crossed-leg test
- confirm by MRI
- treat with longterm semirigid support (plastic splint)
Fractures (associated)
5th metatarsal
- Jones fracture (proximal diaphysis of 5th metatarsal) - high likelihood of non-union.
Refer.
- avulsion of peroneal brevis where it inserts in 5th metatarsal: heals very well
- beware displacement -- needs surgery even if only a few mm laterally
- look for hidden talar dome fracture. May need MRI. Osteochondritis dessicans. Usually
orth removes fragment.
- Tillaux fracture: Salter III fracture of distal tibial epiphysis
- occurs only in adolescents during time that distal tibial epiphysis is
closing; girls 12-14 and boys 15-18.
- Stress fx: very common. Need bone scan. RARE stress fx femoral neck -- prsnt as groin
pain in runner early sprng trng. Pain on hip rotn. NEEDS PINNED FAST. Pars
Interarticularis stress fx cause back pain (extnsn > flexn) in young dancers.
- "Dead arm syndrome": transnt loss strnth arm due sublxatn shoulder. Need refer
to repair.
- Child with sore elbow: r/o osteochondritis dessicans.
- Persistent tennis elbow: r/o post. osseus nerve entrapment.
- Fx hook of hamate: usually while swinging bat/club. Need to remove broken piece.
- iliotibial band syndrome: runner with tenderness over distal lateral femoral condyle.
- Noble compression test: Pt supine, place thumb over the lateral epicondyle, pt
flex/extend -- look for maximal pain @ 30 degrees of flexion
Francis et al. Jama 249:3.p374: Likely no longer valid.
- coumadin 0.5-3.0 mg/qD for 10 days pre-op to keep PT 1.5-3.0 seconds over control
- coumadin increased post-op to give PT 1.5 times control (3.0-5.0 mg/qD)
- evening after surgery
- continue until ambulatory
Causes
- plantar fascia: fasciitis (common), enthesopathies (achilles tendon calcification in
overweight adolescent males)
- soft tissues: bursitis, etc
- calcaneous: stress fracture (tender on mediolateral compression), Paget's, other
- nerve: tarsal tunnel*, abductor digiti quinti muscle nerve entrapment*, S1 radiculopathy
* Tinel's sign positive - percussion of medial aspect of heel causes pain or
paresthesia
Plantar fasciitis
Can be very hard to treat, if initial interventions fail (8 week trial!) refer to
podiatrist or interested orthopod.
- good shoes, not barefoot walking
- heel cup (works better than it should) or heel lift
- stretching exercises of achilles tendon (tight/short tendon stresses
the fascia more -- wonder if moderately heeled shoes help?)
- shoe orthotics
- steroid injection (rupture risk)
- aircast: excellent mobile ankle splint ($35-40). USE FOR ALL ANKLE "SPRAIN".
- BCB splint: good short-term splint for medial collateral ligamentous tears. ($50)
- Bledsoe splint: post-op for anterior cruciate tears ($350-450)
- knee immobilizer: good ER measure pending eval. TEN DAY "WINDOW" FOR LIGAMENT
REPAIR.
- back brace: Raney flexion jacket
- Lightweight Oxford style soft leather, high toe box, extra depth, deep inlay, arch
support, relief area for distal toe, molded plastizote insert for metatarsal pad. (@
$250.00)
- Cotton socks. Cornstarch if will wash feet reg.
- diabetic ankle ulcer: UNNA boot preparations good -- calamine soaked bandage wrap.
Change q 5-7 days (less edema, drying)
See Bisphosphonates Safety and
Efficacy in the Treatment and Prevention of Osteoporosis - May 1, 2000 - AFP. Long
term safety of the biphosphanates is unknown -- use only when indicated.
| therapy |
osteoporosis |
Paget's |
notes |
| ERT, HRT |
x |
|
|
| Alendronate (Fosamax) |
x |
x |
- esophageal problems. biphosphonate
- best evidence and track record.
|
| Calcitonin (Miacalcin) |
x |
x |
- nasal spray marketed for osteo only
- only med for acute use, reduces pain
- unclear if can use along with biphosphanate (review literature prior to consideration)
|
| Etidronate (Didronel) |
* |
x |
- oldest med on market. diphosphonate. few adverse effects, but wasn't all that effective
in trials in decreasing fracture rate
- * not labeled for osteo in US but is elsewhere.
|
| Ibandronate |
? |
? |
- in clinical trials, looks promising. biphosphonate
|
| Residronate (Actonel) |
x |
x |
- may have few GI side effects but is a very new drug (2000)
|
- analgesics
- intranasal calcitonin said to decrease pain
Fracture prophylaxis (esp. nursing home)
- Calcium 1.2 gm daily
- Vitamin D 800 IU daily
Author: John G. Faughnan.
The views and opinions expressed in this page are strictly those of the page author. Pages
are updated on an irregular schedule; suggestions/fixes are welcome but they may take
weeks to years to be incorporated. Anyone may freely link to anything on
this site and print any page; no permission is needed for citing, linking, printing,
or distributing printed copies.

